|
Recently we have set up the Warwickshire Vein
Clinic. This is a partnership between three
consultant vascular surgeons (Peter Blacklay, Dan
Higman and myself) who have worked closely over many
years. Our aim is to use the latest techniques
combined with years of surgical experience to
deliver the highest standards in medical and
surgical care in the treatment of veins.
http://www.warwickshireveinclinic.co.uk/default.aspx
General advice for people with veins
There are a number of simple, generally sensible,
steps that you can take that will ease your symptoms
or prevent them from getting worse.
1. Take regular exercise
2. Attain a healthy weight
3. Eat a healthy balanced diet, including plenty of
fibre to prevent constipation
4. Try to avoid long periods of sitting or standing,
particularly at work or whilst travelling
5. When resting, sit with your feet up
6. Avoid very tight clothing
http://hcd2.bupa.co.uk/fact_sheets/html/Varicose_veins.html
Varicose
Veins
Varicose veins are extremely
common and range in severity from minor cosmetic
veins to venous ulcers. A number of treatments
are available and it is possible to treat all
levels of severity.
The bewildering choice of treatments available
reflect the complex range of conditions that are
grouped together as ‘varicose veins’.
Treatments vary from injection sclerotherapy,
light therapy, laser therapy, foam therapy, VNUS
(and other minimally invasive treatments) to conventional
open surgery.
Your surgeon should be fully conversant with the
full range of conditions and modern treatments
that are available. Each patient needs an individual
treatment plan to address his or her particular
problem.
Normal Veins
Blood travels from the
heart to the extremities via the arteries. The
blood returns to the heart via the veins. In a
lying position the blood returns easily to the
heart. In a standing or sitting position blood
has to travel up hill to get back to the heart.
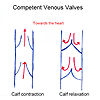
In a normal leg there are a series of one-way
valves which aid the flow back to the heart. Moving
the calf squeezes the calf veins and aids the
return of the blood the heart. This is called
the calf pump.
| |
|
|
Click
on image to enlarge |
 |
|
|
| Normal veins |
Abnormal veins |
| |
|
|
|
Abnormal Veins
However, if the valves are
faulty, when the patient is standing, blood can either flow to the heart or to the feet when the patient is standing.
Long-standing distention of the veins can result
in varicose veins.
Symptoms
Aches and pains (usually towards the end of the
day), which are often worse in hot weather.
Itching, possible flaking skin or eczema.
Swelling
Heavy dragging legs
These symptoms are often worse in women during
their menstrual periods
Signs
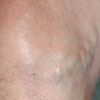
Varicose veins range from
minor cosmetic blemishes through thread or spider
veins to prominent, bulging, unsightly dark blue
veins
Skin changes can occur – pigmentation (haemosiderin
deposition), skin thickening (lipodermosclerosis)
and even ulceration
| |
|
|
Click
on image to enlarge |
 |
|
|
| Varicose Veins |
Substantial
Varicose Veins |
| |
|
|
|
| |
|
|
| |
|
Vulval Varicosity |
Diagnosis and Special
Investigations
Most veins are a result of faulty valves and are
amenable to treatment. However, it is vital to accurately
determine the site of the faulty valves so that
the leaks can be corrected. Failure to deal with
the major leak greatly increases the risk of a recurrence.
Commonly the major leak is in the groin (sapheno-femoral)
or behind the knee (sapheno-popliteal). Occasionally
veins can arise from ‘perforators’ in
the upper or lower leg or more rarely, in women,
from varicose veins in the vulval area. All can
be treated, and treatment will tend to improve both
the symptoms and appearance.
The majority of first time veins can easily be assessed
by clinical examination and a hand held ultrasound
machine (doppler). Recurrent veins, complex veins
or those arising behind the knee, are best assessed
by a simple non-invasive ultrasound technique called
Duplex imaging. All patients with varicose veins
will be assessed in clinic on their first visit
with a portable Duplex machine. I use a SonoSite
MicroMaxx which I find is a robust and portable
machine having used it in the mountains.
http://www.healthimaging.com/index.php?option=com_articles&view=article&id=5452&division=hiit
| |
|
|
Click
on image to enlarge |
| |
 |
|
| |
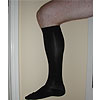
Below knee
support stocking |
|
| |
|
|
|
Treatment Options
| |
|
|
|
| Leave
alone |
|
Most
veins can be left alone but will tend to deteriorate
with time |
|
| |
|
|
| Support
hosiery |
|
Support
hosiery will usually control the symptoms
of the veins (aching discomfort towards the
end of the day). A good fit is essential if
the stockings are to be comfortable and well
tolerated. |
|
| |
|
|
|
| Compression
bandaging |
|
4-layer
compression bandaging is a highly effective
way of treating venous ulcers. Once the ulcer
has been healed, adequate support hosiery
(or venous surgery) is required.
The vast majority of venous ulcers can be
treated in a Community Ulcer Clinic. |
|
| |
|
|
|
| Non-operative
interventions |
|
A
number of treatments have been developed to
treat minor veins, thread veins or spider
veins including injection sclerotherapy, light
or laser treatments.
The basic principle of each treatment is similar,
in that the aim of the treatment is to cause
the blood flow through the small vein to cease.
|
|
| |
|
|
|
| Surgery |
|
The
aim of surgery is to improve both the symptoms
and the appearance of the leg(s) by dealing
with the major leaks and the more minor tributaries.
Surgery is often
performed as a day case either under general,
regional or local anaesthesia. Some bruising
is inevitable and can occasionally be quite
marked. In a small number of patients there
can be some numbness around the wounds or
ankle which usually resolves, but occasionally
persists, but should clear rapidly, and
return to normal activities is quick. Long
haul air travel should be avoided for approximately
6 weeks.
Small scars are inevitable
but they are kept to an absolute minimum.
In a standard ‘high tie strip and
avulsions’, the groin scar, which
is within the bikini line, is normally 2.5-4cms
long. The exit wound at the knee is approximately
1-1.5cms long. Other scars at the site of
the avulsions are very small and sited over
the veins. ‘Pin stripping’ reduces
scars to a minimum and is possible in most
patients. |
|
| |
|
|
|
Thread / Cosmetic Veins
Thread veins are extremely common. They are usually
symptomless, but not always. Thread veins are
often unattractive to the sufferer. A number of
treatments which significantly improve their appearance
are available such as micro injection sclerotherapy,
laser or light therapy.
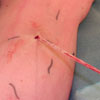
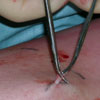
Surgery
Using modern operative techniques it possible
to offer safe conventional surgery through cosmetic
incisions. See photos
| |
|
|
Click
on image to enlarge |
 |
|
|
| Pin Strip |
Vein Hook |
| |
|
|
|
 |
|
|
| Vein Avulsion |
Post Op |
Foam sclerotherapy and EVLT (endovenous laser
treatment)
Over the last couple of years a number of
minimally invasive treatments for varicose veins
have been developed. Both foam and EVLT can be
performed in a treatment room under local
anaesthesia (a bit like going to the dentist)
rather having to be performed in an operating
theatre under a general anaesthetic. This has
advantages in terms of both ease of treatment
and cost over conventional open surgical
treatment. The return to work/sport is much
faster. Long term results remain to be
determined, but the newer techniques appear to
be almost as effective as open surgery but far
less invasive.
The techniques involve identifying the main
veins using ultrasound, and placing a plastic
tube (cannula) under local anaesthesia into the
vein. Using continuous ultrasound guidance it is
possible to seal the major veins using either
glue (foam sclerotherapy) or a laser probe (EVLT).
The glue is an emulsion of a well proven
sclerosant (which has been in use for more than
twenty years) and air. The emulsion shows up
well on ultrasound enabling the operator to see
exactly which veins have been treated. The whole
procedure takes 30-45 minutes and the patient is
able to walk out the treatment room, returning
to normal activities. Firm bandaging and TED (thromboembolic
deterrent) stockings are worn for the first
week, and TED stockings alone for the next week.
NICE Guidelines for foam sclerotherapy 2007:
http://www.nice.org.uk/nicemedia/pdf/IPG314PublicInfo.pdf
NICE Guidelines for EVLT 2004:
http://www.nice.org.uk/nicemedia/pdf/IPG052publicinfo.pdf
New minimally-invasive techniques offer an
effective alternative to open surgery. However
costs and long term results remain issues that
should be discussed.
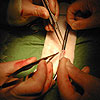
Complex Venous Surgery
Occasionally complex venous
reconstructions are necessary. The picture below
was taken during a kidney transplant. The renal
vein on the donated kidney was too short and it
was necessary to reconstruct an extra length of
vein using the recipient’s own long saphenous
(leg) vein. A metal mandrill is used as a template.
| |
|
|
Click
on image to enlarge |
| |
 |
|
| |
|
|
|
| |
|
|
|
Venous Ulcers
Venous ulcers are the result of years of venous
hypertension. This can be caused by problems in
either the deep veins (previous DVT), the superficial
veins or a combination of both. It is important
to establish the correct diagnosis at an early stage,
since there are a number of other conditions that
can mimic the condition. An assessment of the arterial
supply to the legs and the venous drainage from
the legs is vital. Other factors such as diabetes,
peripheral neuropathies, infection, trauma, cancer
(squamous), and other rarer causes need to be considered.
Adequate compression will heal the majority of venous
ulcers. This can be applied in the form of 4-layer
compression bandages. Once the ulcer is healed,
compression hosiery (at least 20-25mmHg) should
maintain healing.
Venous surgery may be appropriate in some cases.
'MOST VENOUS ULCERS CAN
BE HEALED'
|
|
